TMD

Temporomandibular joint disorder, or dysfunction, (TMD) is a common condition that limits the natural functions of the jaw, such as opening the mouth and chewing.
TMD is often incorrectly referred to as simply “TMJ,” which represents the name of the joint itself and not the disorder.
Its causes range from poor posture, chronic jaw clenching, and poor teeth alignment, to fracture or conditions such as lockjaw, where the muscles around the jaw spasm and reduce the opening of the mouth. Physical therapists help people with TMD ease pain, regain normal jaw movement, and lessen daily stress on the jaw.
What Is Temporomandibular Joint Disorder?
Temporomandibular joint disorder (TMD) is a common condition that limits the natural function of the jaw, such as opening the mouth and chewing, and can cause pain. The temporomandibular joint (TMJ) is a hinge joint that connects your jaw to your skull in front of your ear. The TMJ guides jaw movement and allows you to open and close your mouth and move it from side to side to talk, yawn, or chew. TMD can be caused by:
- Bad posture habits. One of the reasons TMD is so common is because many of us spend a great deal of time sitting at a desk, where we often hold our heads too far forward as we work. But there are many other kinds of bad posture. Sitting in the car for a long commute, working at a checkout station, always carrying your child on the same hip—all can place the head in an awkward position and cause jaw problems. The "forward head position" puts a strain on the muscles, disk, and ligaments of the TMJ. The jaw is forced to "rest" in an opened position, and the chewing muscles become overused.
- Chronic jaw clenching ("bruxism"). Many people clench their jaws at night while they sleep, usually because of stress. Some clench their teeth throughout the day as well, especially when dealing with stressful situations. This puts a strain on the TMJ and its surrounding muscles.
- Problems with teeth alignment ("malocclusion"). If your teeth are positioned in an unusual way, greater stress is placed on the TMJ when performing everyday jaw motions, such as chewing.
- Fracture. In a traumatic accident involving the face or head, a fracture to the lower jaw may result and cause TMD. Even when the fracture is fully healed, TMJ stiffness and pain may remain.
- Surgery. Individuals may experience a loss of TMJ mobility and function following certain kinds of surgery to the face and jaw.
- Trismus ("lockjaw"). This condition—where the jaw muscles spasm and the jaw cannot be fully opened—can be both a cause and a symptom of TMD. Other causes of trismus include trauma to the jaw, tetanus, and radiation therapy to the face and neck.
- Displacement of the disc or soft-tissue cushion located between the ball and socket of the TMJ, which causes popping or clicking of the jaw and, frequently, pain.
- Arthritis in the TMJ.
How Does It Feel?
The symptoms of TMD can be temporary or last for years. Jaw pain is the most common symptom.
CAUTION: Jaw pain also can be a symptom of heart attack. Seek medical care immediately if jaw pain is accompanied by: Chest pain, Shortness of breath, Dizziness, Left arm pain, Numbness in the left arm, Nausea
TMD can cause the jaw to lock or get stuck in a certain position. You may experience headaches, feel pain when chewing certain foods, or have difficulty fully opening your mouth.
TMD symptoms include:
- Jaw pain
- Jaw fatigue
- Difficulty opening your mouth to eat or talk
- Ringing in your ears
- Dizziness
- Headache
- Popping sounds in your jaw
- Neck pain
- Locking jaw
How Is TMD Diagnosed?
To identify the cause of your symptoms, a Rose Physical Therapy expert in TMD will:
- Review your medical history, and discuss any previous surgery, fractures, or other injuries to your head, neck, or jaw.
- Ask you to describe your pain, including headaches, and observe any pain patterns in the neck and TMJ.
- Conduct a physical examination of your jaw and neck, including the soft tissue and muscles in the area.
At Rose, your physical therapist will evaluate your posture and observe how your cervical spine, the upper portion of your spine, situated in your neck, moves. Your physical therapist will examine your TMJ to find out how well it functions and whether there are any abnormalities in your jaw motion.
How Can a Physical Therapist Help?
At Rose your physical therapist can help you restore the natural movement of your jaw and decrease your pain. Based on your condition, your physical therapist will select treatments that will work best for you. Your treatments can include:
Posture Education. If you sit with your head in an increased forward position, you are placing greater strain on the muscles beneath your chin, causing the lower jaw to pull back and the mouth to be in an open position even when resting, increasing stress on the TMJ. You also might be overworking the jaw muscles to force the jaw closed so your mouth isn't open all the time. Your physical therapist will teach you to be aware of your posture so that you can improve the resting position of your jaw, head, neck, breastbone, and shoulder blades when you're sitting and walking.
Neck and Upper Back Symptoms. If these muscles are involved, these would also be included in your treatment plan because they are often incorporated in causing jaw pain.
Improving Jaw Movement. Physical therapists at Rose use skilled hands-on techniques (manual therapy) to gently increase movement and relieve pain in tissues and joints. Your Rose physical therapist may use manual therapy to stretch the jaw in order to restore normal joint and muscle flexibility or break up scar tissues ("adhesions") that sometimes develop when there is constant injury. A Rose physical therapist may also use dry needling to help release muscle trigger points.
Your physical therapist at Rose will teach you special "low-load" exercises that don't exert a lot of pressure on your TMJ, but can strengthen the muscles of the jaw and restore a more natural, pain-free motion.
Special Pain Treatments. Your pain symptoms can be addressed with stretching, exercises, neuromuscular re-education, and methods you would use for any other joint.
Breathing. Breathing issues and shortness of breath, tendency to mouth breathe during exercise or at night, snoring, sleep apnea, clicking and popping of the jaw, are often associated with TMD. Rose Physical Therapy group considers breathing treatments as one of our specialties, something unique amongst physical therapists in the Washington, DC region.
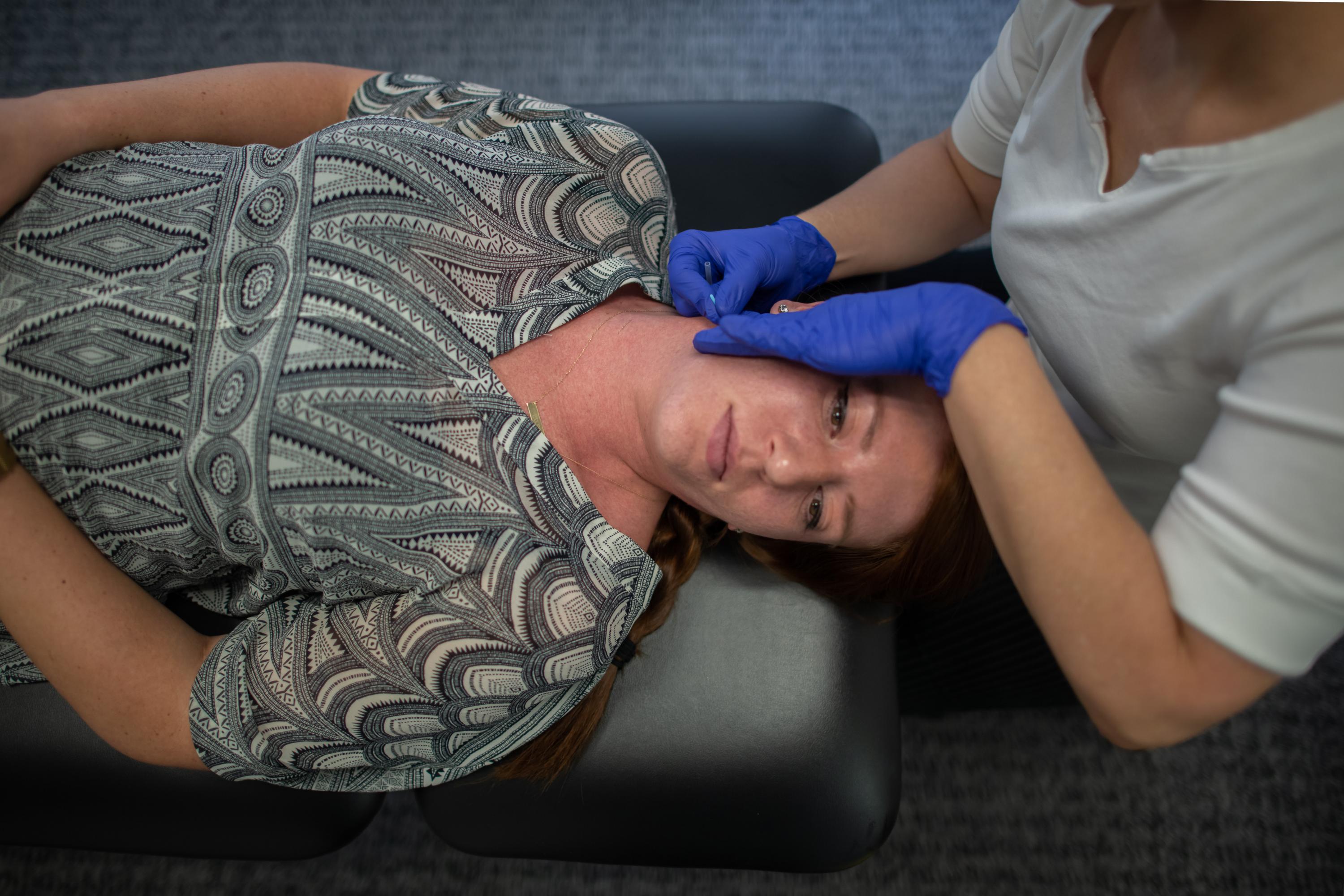
Trigger Point Dry Needling. Dry needling of the face, neck, back and other associated muscles can be used to treat TMD. Rose Phyiscal Therapists are uniquely qualified to implement dry needling as part of your treatment plan for TMD, as dry needling the face is an advanced skill which Rose therapists are certified to perform.
Some considerations for Invisiline and/or Night Guards for Treatment of TMD
It is important to know that TMD is a muscular issue and although invisiline and night guard are commonly offered as a solution, usually by dentists. While these can sometimes be effective, invisline and/or night guards are typically not sufficient to solve the issue of TMD and are often an incomplete treatment. It is important to address the muscular issues associated with TMD, which is why TMD is effectively treated by physical therapy.
Rose Physical Therapy is here in Washington, DC to help!
If you are experiencing pain with TMD, please reach out to make an appointment with one of our jaw and breathing specialists. Physical Therapists at our downtown Washington DC location between Dupont Circle and Farragut Square, or our office near Navy Yard and Capitol Riverfront just a few blocks from Capitol Hill in Washington, DC can get you on the right path for recovery!